 In migraine without aura, the suggestions are that cortical depression may occur in areas where depolarization is not consciously perceived, such as the cerebellum. The cortical spreading depression of Leão, a propagating wave of neuronal and glial depolarization that initiates a cascade, is hypothesized to cause the aura, activate trigeminal afferents, and alter the hematoencephalic barrier permeability by activating brain matrix metalloproteinases. This pathway can, therefore, explain the cortical depression (which establishes the aura) and the latter prolonged activation of trigeminal nociception (which leads to headache). This causes a series of cortical, meningeal, and brainstem events, provoking inflammation in the pain-sensitive meninges and resulting in headaches through central and peripheral mechanisms. There is activation of trigeminal afferents by neuronal pannexin-1 mega channel opening and subsequent activation of caspase-1, followed by the release of proinflammatory mediators, activation of NF-kB (nuclear factor kappa-B), and spreading of this inflammatory signal to trigeminal nerve fibers around vessels of the pia mater. Nowadays, the suggestions pose that multiple primary neuronal impairments lead to a series of intracranial and extracranial changes that cause migraines. Some of the most understood concepts are described in this section.Īccording to the older vascular theory of migraine, headache is produced by vasodilation and aura by vasoconstriction, but this theory is no longer viable. Īlthough not fully understood, pathogenesis involves multiple components of both the peripheral and central nervous systems. Moreover, it is considered the second major cause of disability after back pain with respect to years of life lived with disability. 
Its prevalence increases in puberty but continues to increase until 35 to 39 years of age, decreasing later in life, especially after menopause. It is consistently the fourth or fifth most common reason for emergency visits accounting for an annual 3% of all emergency visits. There is a reported risk of 40% if one parent has a history of migraine, which increases to 75% when both parents have a migraine history. It is ranked as the second leading cause of disability worldwide. 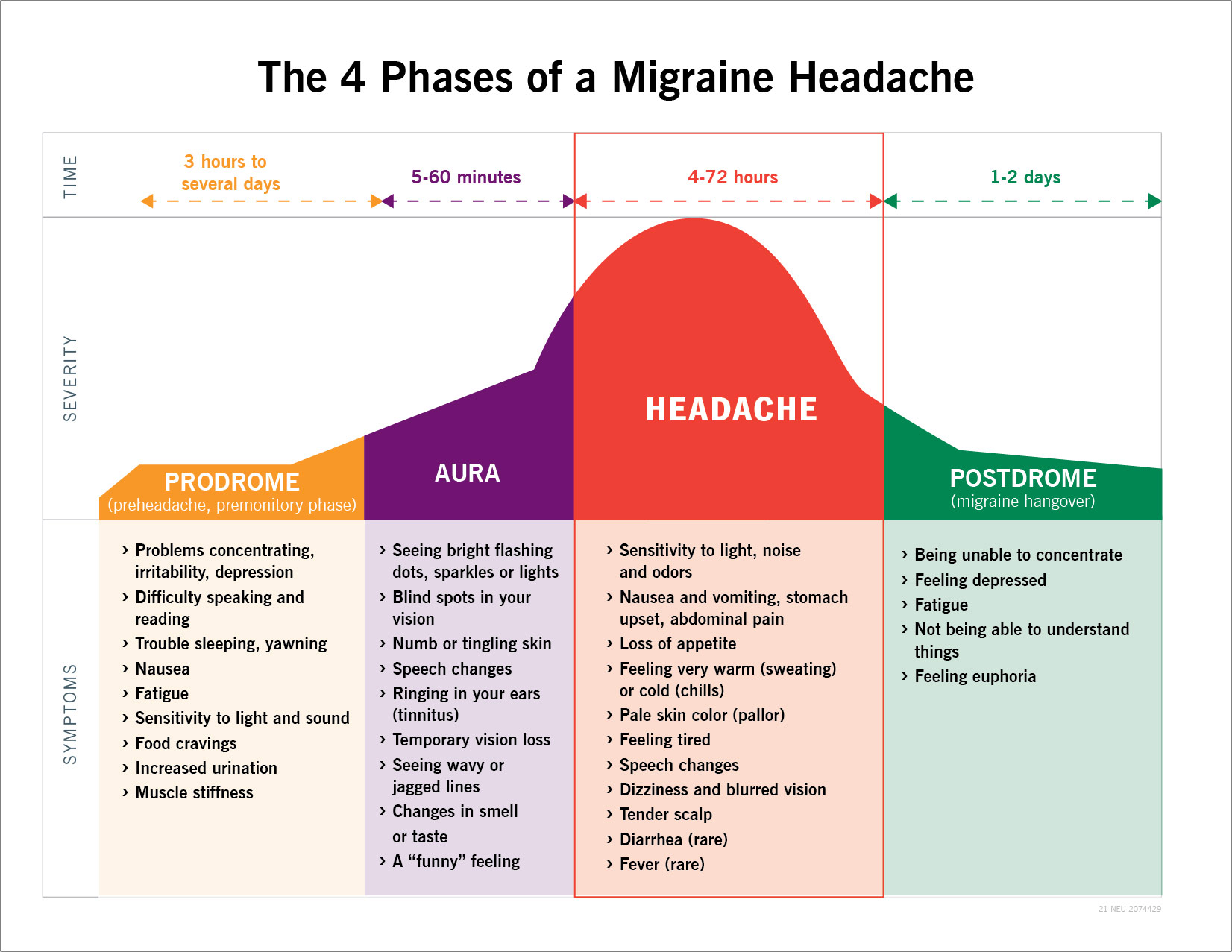
The adjusted prevalence of migraine is highest in North America, followed by South America, Central America, Europe, Asia, and Africa. Among children, it tends to happen more in girls than boys. Migraine is highly prevalent, affecting 12% of the population, attacking up to 17% of women and 6% of men yearly. Some are probable contributing factors, while others are only possible or unproven. 
A retrospective study found that 76% of the patients reported triggers. Withdrawn or exposure to several factors contribute to the development of migraine headaches. Hereditary endotheliopathy with retinopathy, nephropathy, and stroke Hereditary infantile hemiparesis, retinal arteriolar tortuosity, and leukoencephalopathy Retinal vasculopathy with cerebral leukodystrophy is angiopathy by C-terminal frame-shift mutations in TREX1 (three prime repair exonuclease 1) presents almost 60% of the cases. Ĭerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy) angiopathy by autosomal dominant inheritance, caused by mutations in the NOTCH3 gene (notch receptor 3) on chromosome 19 that can present migraine with aura (prodrome in 80%) in nearly 50% of carriers. It is a syndrome of mitochondrial encephalomyopathy, lactic acidosis, and stroke-like episodes, a multisystemic disorder by maternal inheritance that can present recurrent migraine headaches. 
Mutations in the SLC4A4 (solute carrier family four member 4) gene have also been associated with familial forms of migraine. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
